Original Studies
AIM: to assess proliferation and migration of keratinocytes at the nonhealing edges of neuropathic wounds.
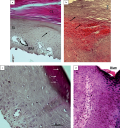
MATERIALS AND METHODS: 25 patients with neuropathic ulcers and 5 patients without diabetes with decubitus were enrolled. Diabetic foot (DF) patients were underwent to standard treatment including debridement, atraumatic dressing, offloading, antibacterial therapy if it needs. Severity of peripheral neuropathy was assessed according to the NDS scale. Histological (hematoxylin and eosin) and immunohistochemical (Ki-67 , α7nAChR markers) examination of wound edge were done during treatment (0, 10, 24 days).
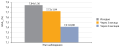
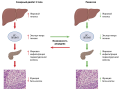
RESULTS: All patients have severe neuropathy according to NDSm (>8). The average size of DF ulcers before and on 10th day of treatment was of 4 cm2 and 2,5 cm2, respectively (p<0,004). Neuropathic ulcers were characterized by hyperproliferative epidermis. Mitotically active keratinocytes reside throughout the suprabasal layers. Ki-67 expressed all layers of the epidermis, but a greater staining density was detected in the basal layer. The density of a7nAChR-positive cells increased from 0 to 24 days (p=0,031).
THE CONCLUSION: The data shows that neuropathy is one of the possible mechanisms of keratinocyte cell cycle disruption: proliferative activity and ability to migrate. Identification of new signaling pathways regulating the physiological repair of tissues and the study of their disorders in diabetes mellitus opens the prospect of developing an optimal therapeutic strategy.
BACKGROUND: The relevance of the study is justified by the fact that in recent years, the original insulin preparations have been replaced with biosimilars in the regions of the Russian Federation, but there are currently few studies describing the use of insulin biosimilars in children with type 1 diabetes mellitus (DM1), both in domestic and foreign sources.
AIM: To evaluate the efficacy and safety insulin therapy with RinFast® (GEROPHARM LLC, Russia) as bolus therapy in combination with long-acting insulin and as monotherapy in an insulin pump in children with DM1 in real clinical practice.
MATERIALS AND METHODS: The dynamics of HbA1c after 3 and 6 months, the change in daily insulin requirements, the fre quency of episodes of postprandial hyper- and hypoglycemia, adverse reactions at injection sites, the number of patients who reached the target values of HbA1c in children with DM1 who received RinFast® at least 6 months after the original analogue of insulin aspart were evaluated.
RESULTS: The study was conducted in 50 children with DM1 from 1 to 18 years old (average age 9.8±4.6 years), with a duration of DM1 of more than 1 year (average duration 3.5±2.1 years), who had glycated hemoglobin (HbA1c) at the beginning of follow-up of no more than 9.5% and received biosimilar RinFast® for at least 6 months after the transfer from the original analogue of insulin aspart. Basic bolus insulin therapy in 36 children was carried out using multiple injections of insulin (MII), in 14 — continuous supply of insulin (NPI) using an insulin pump. The study resulted in HbA1c levels comparable to the baseline 3 and 6 months after the start of therapy with the RinFast® biosimilar (p=0.05), no changes in the daily insulin requirement (p=0.05) and no increase in the frequency of episodes of postprandial hyper- (p=0.05) and hypoglycemia (p=0.05) and adverse events (p=0.05). High adherence to treatment with the RinFast® biosimilar was noted.
CONCLUSION: The results obtained indicate the absence of a clinically significant deterioration in glycemic control indicators after the transfer of children with DM1 to therapy with the RinFast® biosimilar, which makes it possible to use it safely and effectively in this category of patients.
BACKGROUND: It is important to evaluate the effect of androgen replacement therapy on glycemic control.
AIMS: Assessment of the effect of transdermal testosterone therapy on glycemic control in men with hypogonadism and T2DM.
MATERIALS AND METHODS: The prospective, comparative study included 300 men aged 55[49;61] years: men receiving both glucose-lowering therapy (GLT) and transdermal testosterone; and patients receiving only GLT. Observation period 1 year. A medical history, a questionnaire for symptoms of androgen deficiency, and measurement of total testosterone and glycated hemoglobin were carried out. Groups were compared using nonparametric methods.
RESULTS: Patients receiving androgen replacement therapy in combination with GLT at both 6 and 12 months from the moment of inclusion in the study, they had a statistically significantly higher level of total testosterone and less severity of symptoms of androgen deficiency. When assessing the magnitude of changes in the studied parameters, it was found that patients receiving testosterone replacement therapy (TRT) were characterized by a statistically significantly more pronounced decrease in the level of glycated hemoglobin (average difference 0,3%). In 29 (20,4% (95% ДИ 13,8–27,0)) men who received only GLT, hypogonadism was eliminated. In 3 patients from the TRT group, a pathological increase in the level of total blood PSA was observed, and therefore TRT was discontinued. An increase in hemoglobin above the reference value (>172 g/l) was detected in 8% and 1,3% of men on TRT and without correction of hypogonadism, respectively, p=0,011.
CONCLUSIONS: The combination of transdermal TRT and GLT has a positive effect on glycemic control, which is manifested by a decrease in glycated hemoglobin to a greater extent than when using GLT alone. Normalization of testosterone levels leads to a decrease in the symptoms of androgen deficiency, which is accompanied by an improvement in quality of life. Elimination of hypogonadism only with GLT is possible in a small number of cases.
BACKGROUND: Time in range (TIR) is a promising indicator of glycemic control used for evaluation of continuous glucose monitoring (CGM) for patients with diabetes mellitus (DM). The current problem is the assessment and prediction of TIR for patients who use self-monitoring of blood glucose (SМBG) corresponding low CGM availability for the majority of diabetic patients.
AIM: To develop a predictive model of TIR for patients with T1DM based on data of the experimental mobile application.
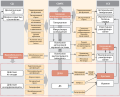
MATERIALS AND METHODS: An analysis of 1253 professional CGM profiles of patients with T1DM was performed. On the base of included records, TIR(CGM) was calculated and training models of 7-point SMBG profiles were generated. SMBG profiles’re loaded into the developed experimental mobile application that calculated standard glycemic control parameters. The dataset was divided into main and test samples (80 and 20%). For the main sample, the following methods’re used to develop predictive models: simple linear regression (SLR), multiple linear regression (MLR), artificial neural network (ANN). The effectiveness of the developed models was assessed on the test sample with the calculation of the mean absolute error (MAE), the root mean square error (RMSE).
RESULTS: The 568 CGM profiles’re included in the study. TIR in the main group (n=454) — 45 [33; 65]%, in the test group (n=114) — 43 [33; 58]%. The most significant predictors of the regression models were the derived TIR (dTIR), p<0,001; derived time below range level 1 (dTBR1), p<0,001; standard deviation of blood glucose (SD), p=0,007. Determination coefficient for SLR (predictor: dTIR) — 0,844; for MLR (predictors: dTIR, dTBR1, SD) — 0,907. ANN multilayer perceptron models with two and one hidden layers’re developed, with the RMSE on the validation set 4,617 and 6,639%, respectively. The results of the forecast efficiency on the test sample were: dTIR: MAE — 6,82%, RMSE — 8,60%; SLR: MAE — 5,66%, RMSE — 7,34%; MLR: MAE — 4,18%, RMSE — 5,28%; ANN (2 layers): MAE — 4,14%, RMSE — 5,19%; ANN (1 layer): MAE — 4,44%, RMSE — 5,52%.
CONCLUSION: ANN with two hidden layers and MLR demonstrated the best ability for TIR prediction. Further studies are required for clinical validation of developed prognostic models.
BACKGROUND: The incidence of diabetes mellitus (DM) both in the Russian Federation and in the world has been steadily increasing for several decades. Stable population growth and current epidemiological characteristics of DM lead to enormous economic costs and significant social losses throughout the world. The disease often progresses with the development of specific complications, while significantly increasing the likelihood of hospitalization. The creation and inference of a machine learning model for predicting hospitalizations of patients with DM to an inpatient medical facility will make it possible to personalize the provision of medical care and optimize the load on the entire healthcare system.
AIM: Development and validation of models for predicting unplanned hospitalizations of patients with diabetes due to the disease itself and its complications using machine learning algorithms and data from real clinical practice.
MATERIALS AND METHODS: 170,141 depersonalized electronic health records of 23,742 diabetic patients were included in the study. Anamnestic, constitutional, clinical, instrumental and laboratory data, widely used in routine medical practice, were considered as potential predictors, a total of 33 signs. Logistic regression (LR), gradient boosting methods (LightGBM, XGBoost, CatBoost), decision tree-based methods (RandomForest and ExtraTrees), and a neural network-based algorithm (Multi-layer Perceptron) were compared. External validation was performed on the data of the separate region of Russian Federation.
RESULTS: The best results and stability to external validation data were shown by the LightGBM model with an AUC of 0.818 (95% CI 0.802–0.834) in internal testing and 0.802 (95% CI 0.773–0.832) in external validation.
CONCLUSION: The metrics of the best model were superior to previously published studies. The results of external validation showed the relative stability of the model to new data from another region, that reflects the possibility of the model’s application in real clinical practice.
Review
In this review, information is presented within the triad: obstructive sleep apnea/hypopnea syndrome (OSA), glycemic variability, and cardiac arrhythmias in patients with type 2 diabetes mellitus (DM2). Epidemiological aspects, pathogenetic relationships, possible instrumental and laboratory diagnostic methods, as well as approaches to personalized therapy are analyzed. Research is being actively conducted in certain areas of the designated triad, however, no studies have been found that include simultaneous monitoring of indicators reflecting these disorders in patients with DM2. Many issues are still controversial. Sleep disturbances in patients with DM2 are actively studied, but more often questionnaires are used for diagnosis, rather than instrumental methods. There is insufficient data examining the effect of hypoxia on the progression of complications in patients with DM2. Rhythm disturbances are being actively studied in patients with DM2 in combination with various cardiological problems. Of greatest interest is the study of rhythm disturbances in patients with DM2 without concomitant comorbid conditions of the cardiovascular system, in order to identify early signs of diabetic cardiovascular autonomic neuropathy and cardiomyopathy, as well as additional early risk factors for the development and progression of cardiovascular diseases. Most of the studies are devoted to the study of the association of OSA and various arrhythmias in cardiac patients. However, there is no data on the combined effect of glycemic variability and OSA on the development of cardiac arrhythmias in patients with DM2. Additional studies are needed to identify the features of the effect of OSA on cardiac arrhythmias in patients with DM2.
Last time there are a lot of date, published systematic reviews and meta-analyses about relationship between eating behavior and incidence type 2 diabetes. It is known that more than 80% of cases of type 2 diabetes are associated with obesity. In this regard, the nutritional factor is of particular importance in the formation of treatment goals for patients with type 2 diabetes. Today, the disease is no longer a sentence, because achieving remission of type 2 diabetes is possible with the help of nutritional correction. The results of studies shown that a significant decrease in body weight is a predictor of remission of type 2 diabetes. However, the question of the best dietary recommendations for patients with type 2 diabetes remains open. Various dietary patterns (Mediterranean, paleo diet, DASH system, etc.) contribute to the improvement of glycemia, however, there is not enough data indicating a regression of symptoms of type 2 diabetes. In all likelihood, achieving remission is possible only with a significant reduction in daily caloric intake. The ketogenic diet, especially popular in recent times, also improves glycemic control. At the same time, according to the results of a meta-analysis, carbohydrates from whole grains and cereal fibers should not be neglected, because this category of products helps reduce the risk of developing diabetes.
Patients with type 2 diabetes mellitus (T2DM) are at high risk of adverse outcomes in coronavirus infection (COVID-19). Despite the gradual resolution of the pandemic, new strains of the virus are emerging, characterized by high contagiousness, and the risk of infection becoming a seasonal disease is increasing. In this connection, the issue of identifying risk factors that aggravate the course of COVID-19 in patients with T2DM, including the role of initial hypoglycemic therapy, remains relevant.
The review presents and systematizes up-to-date information (according to randomized clinical trials and meta-analyses) on the effect of outpatient and inpatient use of metformin and innovative hypoglycemic drugs (glucagon-like peptide-1 receptor agonists, sodium-glucose cotransporter-2 inhibitors, dipeptidyl peptidase-4 inhibitors) on the course and outcome of COVID-19 in patients with T2DM. At the same time, the potential mechanisms of the pathogenetic effect of drugs on the course of COVID-19, positive and negative aspects of their administration are described.
Case report
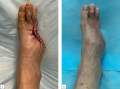
The article presents the result of our own observation of the patient with a poor control of type 2 diabetes mellitus (DM) for a long period, complicated by obliterating atherosclerosis of the arteries of the lower extremities, Menckeberg’s sclerosis and chronic ischemia threatening loss of the lower extremity (CLLI). A feature of the clinical manifestation are complications associated with potentially regional (angiosomal) ischemia of the foot, as well as variant anatomy, represented by hypoplasia of the vascular lower leg in the patient. The clinical consequences of vascular calcification due to long-term decompensation of carbohydrate metabolism and the development of diabetic distal polyneuropathy (DDP) led to falsely high values of the cuff test in the patient. Disadvantages of non-invasive methods for diagnosing limb ischemia and advantages of the complex application of tests for diseases of the arteries of the lower extremities are discussed. Using WIFI classification according to the degree of ulceration, the degree of ischemia, and the degree of infection on the foot (Wound, Ischemia and Foot Infection), the tactics of managing the patient are presented. The important role of ultrasonic duplex scanning (USDS) in the visualization of the arteries of the legs and feet in patients with DM is substantiated. The importance of a multidisciplinary approach in the management of a comorbid patient with type 2 diabetes and CLTI is emphasized.
This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License (CC BY-NC-ND 4.0).
ISSN 2072-0378 (Online)